Targeted Therapies
In GeneReviews, a targeted therapy is one that addresses the specific underlying mechanism of disease causation (regardless of whether the therapy is significantly efficacious for one or more manifestation of the genetic condition); would otherwise not be considered without knowledge of the underlying genetic cause of the condition; or could lead to a cure. —ED
Therapeutic phlebotomy is a standard of care for individuals with HFE HC who have either only biochemical evidence of iron overload (i.e., elevated serum ferritin) or clinical manifestations of iron overload (i.e., evidence of end-organ damage including cirrhosis, cardiac failure, skin hyperpigmentation, diabetes, or hypogonadotropic hypogonadism).
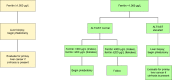
The European Association for the Study of the Liver [2022] suggests phlebotomy therapy for individuals with evidence of iron overload. The HEIRS Study suggested that phlebotomy therapy be started in males with serum ferritin >300 µg/L and in females with serum ferritin >200 µg/L [Adams et al 2005]. In a study of Australian individuals with HFE HC, there was evidence of subjective and objective improvement by reducing serum ferritin levels to <300 µg/L [Ong et al 2017].
Therapeutic phlebotomy (i.e., removal of a unit of blood) is a simple, inexpensive, safe, and effective way to remove excess iron. Each unit of blood (400-500 mL) with a hematocrit of 40% contains 160-200 mg of iron.
The usual therapy is phlebotomy weekly until the serum ferritin is ≤100 µg/L. Twice-weekly phlebotomy may be useful to accelerate iron depletion in individuals with serum ferritin >1,000 µg/L or those with evidence of end-organ damage due to iron overload. Hematocrit or hemoglobin (Hb) concentration should be assessed prior to each phlebotomy. If serum ferritin is very high, serum ferritin measurement should be performed approximately every five to ten phlebotomies. Some persons, especially females, tolerate phlebotomy poorly. In such instances, the interval between phlebotomies should be increased (e.g., every 10-14 days) or phlebotomy volume should be reduced (e.g., 250-300 mL).
Anemia is not a characteristic of HFE HC. In individuals with anemia due to other causes, the Hb concentration at which phlebotomy is not recommended or at which the phlebotomy regimen should be interrupted depends on individual factors including symptoms of anemia, comorbid conditions, age, and ability to perform ordinary tasks and carry out daily activities, while taking into account the relative importance of the procedure. For example, in individuals with severe iron overload, some degree of anemia is acceptable if phlebotomy is tolerated by the individual. In some causes of anemia (e.g., anemia of renal insufficiency), treatment of the underlying anemia with an erythropoiesis-stimulating agent may improve tolerability of phlebotomy. Increasing erythropoiesis will also enhance iron incorporation in erythrocytes.
The serum ferritin concentration is the most feasible and inexpensive way to monitor therapeutic phlebotomy. After serum ferritin is ≤100 µg/L, serum ferritin concentration should be quantified after each additional one or two treatments [Adams & Barton 2010]. On average, males require removal of twice as many units of blood to achieve iron depletion as females.
Maintenance phlebotomy to prevent reaccumulation of excess iron is indicated for males with serum ferritin ≥300 µg/L and for females with serum ferritin ≥200 µg/L [Adams & Barton 2010].
Phlebotomy may decrease fatigue, arthralgias, and hepatic enzyme levels in many individuals and induce regression of liver fibrosis and cirrhosis in some individuals. Conclusive data regarding the favorable influence of therapeutic phlebotomy on quality of life, diabetes, liver cancer risk, or cardiomyopathy is lacking [Prabhu et al 2020]. Therapeutic phlebotomy increases overall survival [Bomford & Williams 1976, Milman et al 2001].
Whether lowering transferrin saturation should be a target of phlebotomy therapy is debatable. Elevated transferrin saturation in HFE HC is caused by increased iron export from macrophages due to hepcidin deficiency and is not a marker of iron overload. Attempting to achieve and maintain low transferrin saturation in individuals with HFE HC may result in iron deficiency and associated adverse manifestations [Barton & Bottomley 2000].
Note: Hb, mean corpuscular hemoglobin (MCH), and mean corpuscular volume (MCV) levels are not targets of treatment in persons with HFE HC.
Erythrocytapheresis is an effective and safe alternative to phlebotomy therapy for individuals with HFE HC, although few facilities can provide erythrocytapheresis, whereas many can provide therapeutic phlebotomy. Fixed-volume erythrocytapheresis results in a faster initial decline in serum ferritin and a reduced number of procedures than phlebotomy therapy, although it does not achieve target serum ferritin levels sooner [Sundic et al 2014]. Reports of treatment duration and total costs of individualized erythrocytapheresis (based on sex, body weight, total blood volume, and hematocrit) in the induction phase of therapy, compared to those of phlebotomy, are variable [Rombout-Sestrienkova et al 2012, Sundic et al 2014]. In the maintenance phase of therapy, individualized erythrocytapheresis reduced the number of procedures required in comparison with phlebotomy therapy but not the total costs per treatment year [Rombout-Sestrienkova et al 2016]. Blood components removed during erythrocytapheresis may be suitable for transfusion. Mild citrate reactions are common with erythrocytapheresis.
Iron chelation therapy to achieve iron depletion is a treatment alternative for individuals who have an elevated serum ferritin concentration and concomitant symptoms of anemia, inadequate venous access, or another circumstance that makes therapeutic phlebotomy or erythrocytapheresis inadvisable, although studies of chelation therapy in individuals with HFE HC are very limited. Oral deferasirox at 10 mg/kg/day was the starting dose for most individuals with HFE HC in two studies [Phatak et al 2010, Cançado et al 2015]. Deferasirox therapy is not appropriate for individuals with advanced liver disease. Subcutaneous deferoxamine was effective in achieving iron depletion in three individuals with HFE HC in whom phlebotomy therapy was not feasible [Nielsen et al 2003].